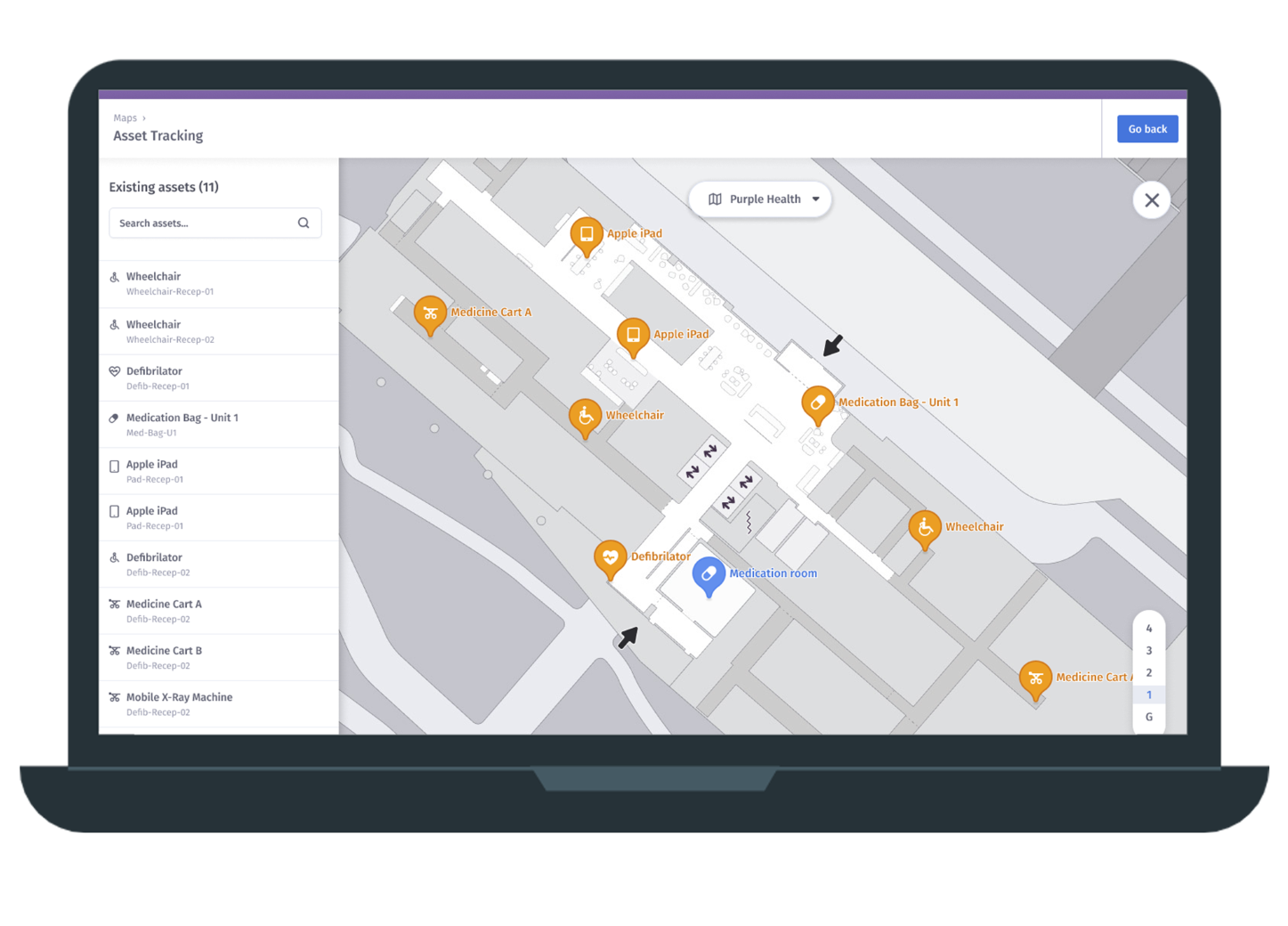
Radar Healthcare report ranks UK second on overall healthcare equalities

Report from Radar Healthcare shows Canada leading the way on overall healthcare equality, with the UK and other northern European Countries making up the rest of the top six.
A new Healthcare Inequalities Report, released by Radar Healthcare, has ranked 35 of the most developed countries around the world, offering a comprehensive insight into which of these countries offers the best healthcare rights to its citizens through their laws and regulations.
The report places Canada, the UK and Norway in the top three for global healthcare equality, with each generally offering fair and equitable access to healthcare for its citizens.
Radar Healthcare’s report also makes reference to a recent Public Policy Projects report, A Women’s Health Agenda: Redressing the Balance, which produced a series of recommendations aimed at improving the design, delivery and outcomes of women’s healthcare.
While the UK places well overall, the report ranks it number 1 for factors relating specifically to women, with Canada coming in second place.
Below is a snapshot of the report’s findings on maternity and paternity leave.
Maternity and paternity leave
The UK lags behind Denmark and Norway on the ‘paid maternity leave’ metric, offering 39 weeks of paid leave and 13 weeks of unpaid leave, compared with 52 weeks of paid leave in Denmark, while Norway offers 49 weeks of paid leave and 59 weeks of unpaid leave.
The report draws key distinction between paid and unpaid maternity leave; a high number of overall weeks of maternity leave may appear impressive but the degree to which this includes paid leave is highly consequential. For example, Italy offers 4 months of paid maternity leave and 17 weeks of unpaid leave, however, leaving a new mother without a salary for 17 weeks places them in a potentially vulnerable situation, perhaps leaving them more reliant on a partner or family for support.
On paternity leave, the UK scores poorly, scoring offering just 14 days of paid leave to new fathers, while Sweden offers 240 days, the Netherlands 182 days and Denmark 168 days. Germany, meanwhile, has no laws mandating employers to offer new fathers paternity leave, either paid or unpaid.
The lower provision of paid paternity leave is a key metric of gender-based healthcare inequality, since less leave for fathers places more of the burden for childcare on mothers, as well as limiting the valuable bonding time between a newborn and their father.
Further to maternity and paternity leave, the report assesses each country’s standing in regard to the following categories:
- The legal age of consent – the age at which a person is considered to be legally competent to consent to sexual acts
- Doctor / patient confidentiality ages – the age a resident can speak confidentially to a healthcare professional without parents/guardians being informed
- Cervical cancer screening – what age they are recommended for women around the world
- Mammogram screening tests – what age they are recommended for women
- Flu vaccines – at what age is this offered to elderly residents around the globe
- IVF treatment age range – how age impacts the chances of becoming a parent via in-vitro fertilisation in different countries around the world
- Cosmetic surgery – at what ages someone can have a cosmetic surgery procedure
- Transgender hormone treatment – at what age do healthcare practitioners in different countries allow transgender patients to start hormone treatment
- Access to birth control around the world – (age requirements/costs/the countries offering free birth control)
- Abortion laws – how they differ across the world
Commenting on the report, Hayley Levene, Head of Marketing at Radar Healthcare, said: “Radar Healthcare partners with organisations such as Public Policy Projects who are learning from experience (both their own and others) to make contributions to the policy debate which address real-world choices on the basis of real-world evidence.
“As a healthcare supplier, Radar Healthcare is passionate about helping to make a difference and delivering improved outcomes. Working with PPP to produce reports such as ‘The Social Care Workforce: averting a crisis’, ‘The Digital Divide: reducing inequalities for better health’ and ‘Integrating Health and Social Care: a national care service’ is vital in helping to drive change and improve some of these health inequalities.
“For example, technology could offer oversight that 80 per cent of patients or healthcare workers themselves are having suicidal thoughts – and this could prompt a process to be followed to tackle it, which will encourage decisions of change.”
To find out more, please visit www.radarhealthcare.com.